When it comes to modern bone repair and orthopedic surgery, innovation is moving beyond metal plates and traditional bone grafts. One material gaining major attention in regenerative medicine is bioactive glass — a scientifically engineered biomaterial that actively supports bone healing rather than simply stabilizing it.
In this SEO-optimized guide, we’ll explain:
- What bioactive glass is
- How it works in bone regeneration
- Its advantages over traditional implants
- Clinical applications in orthopedic surgery
- Why it’s shaping the future of bone healing
What Is Bioactive Glass?
Bioactive glass is a synthetic biomaterial composed primarily of:
- Silicon dioxide (SiO₂)
- Calcium oxide (CaO)
- Sodium oxide (Na₂O)
- Phosphorus pentoxide (P₂O₅)
Unlike ordinary glass, bioactive glass is specifically designed to interact with biological tissue. It was first developed by Larry Hench in 1969 and introduced as 45S5 Bioglass®, marking a breakthrough in bone regeneration technology.
The key difference?
👉 Bioactive glass does not just fill a bone defect — it stimulates new bone formation.
How Bioactive Glass Works in Bone Healing
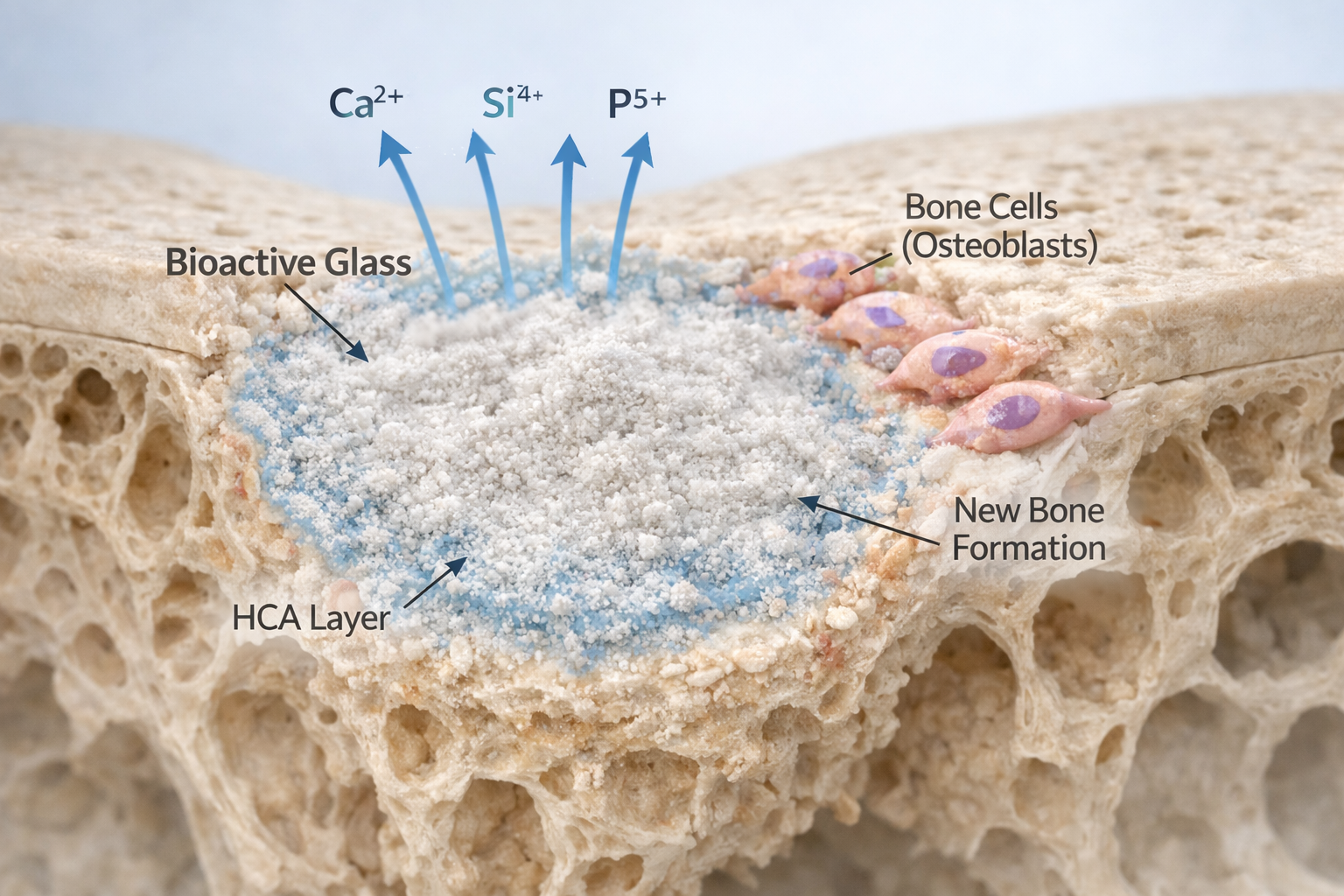
When bioactive glass is implanted into a bone defect, a series of scientifically proven reactions occur:
- Ion Release – The material dissolves slowly in body fluids, releasing calcium and silicon ions.
- Surface Reaction – A hydroxycarbonate apatite (HCA) layer forms on the surface.
- Cell Activation – Osteoblasts (bone-forming cells) attach and multiply.
- Bone Bonding – New bone grows directly onto the material.
This process is called osteostimulation — meaning the material actively promotes bone regeneration.
Unlike traditional materials that provide only structural support, bioactive glass participates in the healing process.
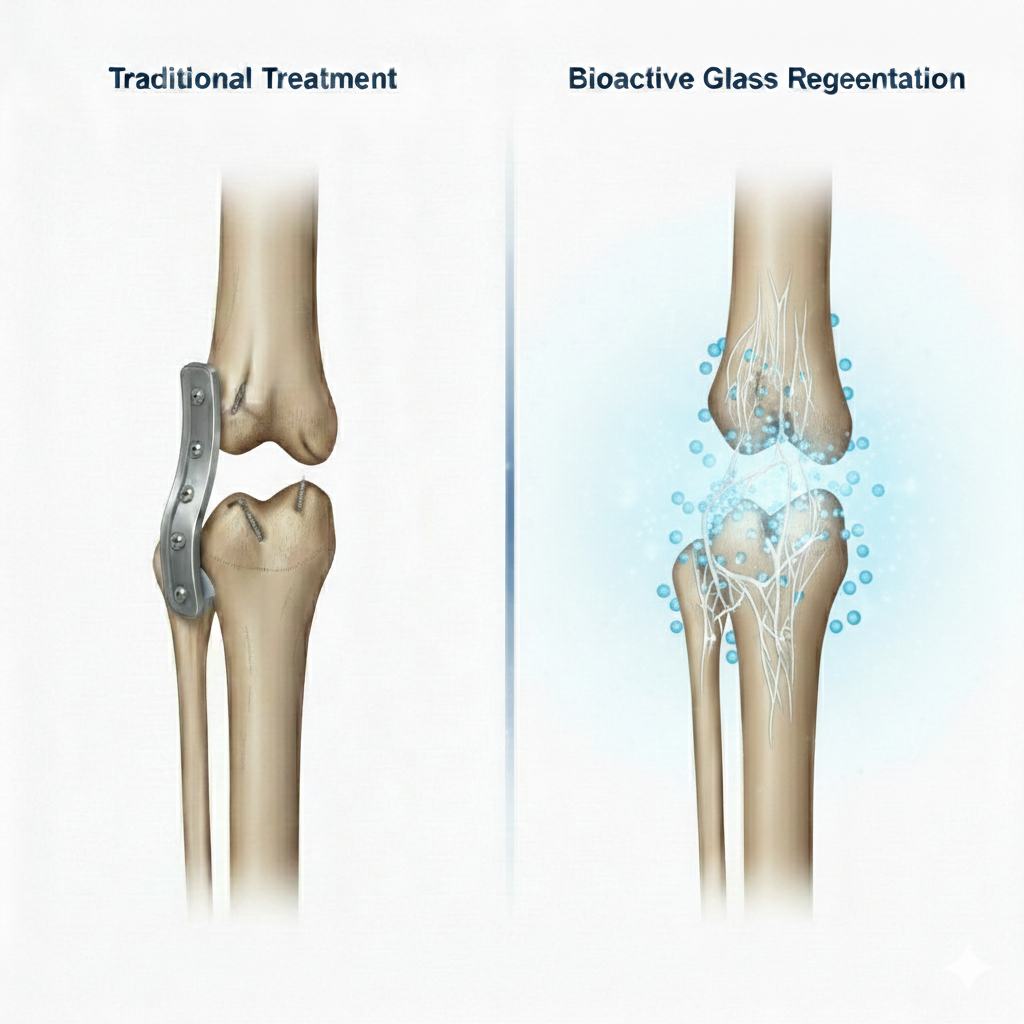
Bioactive Glass vs Traditional Metal Implants
In orthopedic fracture treatment, metal plates and screws are commonly used to stabilize broken bones. While they provide excellent mechanical strength, they are biologically passive.
Traditional Metal Implants:
- Provide structural stabilization
- Do not stimulate bone growth
- Remain permanently unless removed
- May cause stress shielding
Bioactive Glass:
- Stimulates bone cell activity
- Forms a bonding layer with bone
- Gradually dissolves as bone regenerates
- Supports natural healing
💡 Key Difference:
Metal stabilizes. Bioactive glass regenerates.
In many procedures, surgeons combine both — metal for strength, bioactive glass for biological enhancement.
Bioactive Glass vs Hydroxyapatite
Another commonly used bone graft substitute is hydroxyapatite. Both materials bond with bone, but they behave differently.
| Feature | Bioactive Glass | Hydroxyapatite |
| Biological Activity | High (ion release) | Moderate |
| Degradation Rate | Controlled, tunable | Very slow |
| Bone Stimulation | Strong | Primarily conductive |
| Antibacterial Effect | Yes | Minimal |
Bioactive glass is often preferred in cases requiring faster biological response and enhanced bone regeneration.
Clinical Applications of Bioactive Glass in Orthopedics
Bioactive glass is used in several orthopedic procedures:
1. Bone Defect Repair
Used to fill gaps caused by trauma, tumor removal, or infection.
2. Spinal Fusion Surgery
Enhances bone growth between vertebrae.
3. Treatment of Osteomyelitis
Its antibacterial properties help manage bone infections.
4. Revision Joint Surgery
Supports bone regeneration after implant removal.
5. Dental and Maxillofacial Surgery
Improves jawbone and periodontal regeneration.
Benefits of Bioactive Glass in Orthopedic Surgery
Here are the top advantages:
✔ Stimulates Bone Regeneration
Encourages osteoblast activity and faster healing.
✔ Forms Direct Chemical Bond
Creates strong integration with natural bone.
✔ Antibacterial Properties
Reduces infection risk in surgical sites.
✔ Biocompatible and Safe
Decades of research support its clinical safety.
✔ Controlled Degradation
Gradually replaced by natural bone tissue.
Is Bioactive Glass Strong Enough for Load-Bearing Bones?
Pure bioactive glass is brittle and not suitable alone for major weight-bearing applications like femoral fractures.
However, modern advancements include:
- Bioactive glass–polymer composites
- Bioactive coatings on metal implants
- 3D-printed hybrid scaffolds
These combinations provide both mechanical strength and biological stimulation.
Why Bioactive Glass Is the Future of Bone Regeneration
Orthopedic medicine is evolving from passive fixation to active regeneration.
The future focuses on:
- Faster recovery
- Reduced surgical complications
- Lower infection rates
- Improved implant integration
- Regenerative biomaterials
Bioactive glass aligns perfectly with these goals.
Emerging research includes:
- Injectable bioactive glass putty
- Drug-loaded bioactive scaffolds
- Patient-specific 3D printed implants
As regenerative medicine grows, bioactive glass is expected to play an increasingly central role.
Final Thoughts
Bioactive glass represents a major advancement in orthopedic biomaterials. Unlike traditional implants that simply stabilize fractures, this material actively participates in bone regeneration.
If you are researching advanced bone graft materials, regenerative orthopedics, or innovative fracture treatment options, bioactive glass stands out as a scientifically backed and clinically proven solution.
Contact us through Synthera Biomedical social platforms to stay informed about pioneering bioactive glass research and clinical applications. Follow us on Instagram for product launches and research updates. Join the conversation on Facebook to access valuable resources and community news.
References:
1. Redhwi, I., Fallatah, A., & Alshabona, F. (2024). Hydroxyapatite: A comprehensive review of its properties, applications, and future trends. International Journal of Biomedical Materials Research, 12(1), 1–10. https://doi.org/10.11648/j.ijbmr.20241201.11
2. Shi, H., Zhou, Z., Li, W., Fan, Y., Li, Z., & Wei, J. (2021). Hydroxyapatite based materials for bone tissue engineering: A brief and comprehensive introduction. Crystals, 11(2), 149. https://doi.org/10.3390/cryst11020149
3. Hench, L. L., & Paschall, H. A. (1973). Direct chemical bond of bioactive glass-ceramic materials to bone and muscle. Journal of Biomedical Materials Research, 7(3), 25–42. https://doi.org/10.1002/jbm.820070304
4. Liu, W., Cheong, N., He, Z., & Zhang, T. (2025). Application of hydroxyapatite composites in bone tissue engineering: A review. Journal of Functional Biomaterials, 16(4), 127. https://doi.org/10.3390/jfb16040127
5. Hench, L. L. (2013). Chronology of bioactive glass development and clinical applications. New Journal of Glass and Ceramics, 3(2), Article ID30885. https://doi.org/10.4236/njgc.2013.32011
6. Filip, D. G. (2022). Current development in biomaterials—Hydroxyapatite and Bioglass for applications in biomedical field: A review. Materials. https://www.mdpi.com/1996-1944/13/4/248
7. Nascimento Santos, J. V. do, Sousa de Moraes, P. W., Pereira, M. N., Costa Leite, J. V., Pinto Magalhães, G. de A., Capehart, K., & Lima, R. B. W. E. (2025). Bioactive glass products for the treatment of dentin hypersensitivity: a scoping review. Clinical Oral Investigations, 29(10), 464. https://doi.org/10.1007/s00784-025-06516-w
8. Shi, H., Zhou, Z., Li, W., Fan, Y., Li, Z., & Wei, J. (2021). Hydroxyapatite based materials for bone tissue engineering: A brief and comprehensive introduction. Crystals, 11(2), 149. https://doi.org/10.3390/cryst11020149
9. Hench, L. L. (2006). The story of Bioglass®. Journal of Materials Science: Materials in Medicine, 17(11), 967–978. https://doi.org/10.1007/s10856-006-0432-4